How Long Is The Actual Surgery For Trochanteric Bursitis Wirh Gluteus Repairs
Abstract
Purpose
Surgery for greater trochanteric pain syndrome (GTPS) may exist indicated for cases refractory to conservative measures. We aim to evaluate patient reported outcomes and adverse events following surgery.
Methods
Postal questionnaires were used to evaluate a consecutive series of 61 bursectomy and gluteal fascia transposition (GFT) procedures. Study outcomes were Oxford hip score, satisfaction score, visual analogue score, pain lying on the affected side, and the duration of pain relief subsequently surgery.
Results
We received responses regarding 52 procedures at a median of 34 months follow-up; twoscore% of cases of GTPS occurred post-obit THA. Nosotros observed a bimodal distribution of satisfaction scores. The early post-operative complication charge per unit was xiii%; an additional 7 cases (12%) required further surgery at a after engagement. Idiopathic GTPS had significantly ameliorate post-operative satisfaction than GTPS following THA, 87.five vs. 37.five (p = 0.006); Oxford hip scores, 35 vs. xv (p = 0.015); and visual analogue scores, 20 vs. 73 (p = 0.005).
Determination
We observed overall poor outcomes, significant complications and concerning reoperation rates. Cases with previous joint replacement were associated with the worst outcomes.
Introduction
Greater trochanteric pain syndrome (GTPS) is a clinical diagnosis of disabling hurting localised over the lateral attribute of the hip [one, 2] worsened by lying on the affected side. What was once thought of, and is still sometimes referred to, as 'trochanteric bursitis' is now understood to involve a wider number of structures surrounding the greater trochanter including tendinopathy and micro-trauma to the gluteus medius and minimus tendons [3] (Fig. 1), often without classic signs of inflammation implied by the term 'bursitis' [4].
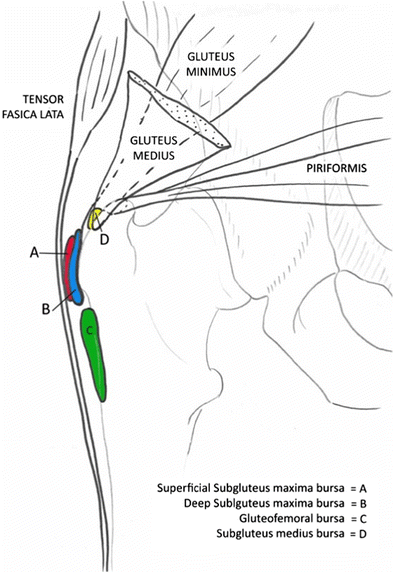
Posterior aspect of the beefcake around the greater trochanter, showing structures commonly implicated in greater trochanteric pain syndrome
The prevalence of GTPS in the full general population ranges from 10 to 25% [5]. When participants of an observational study aged betwixt l and 79 years were specifically questioned and examined for features of GTPS, the prevalence was identified at 17.6% [4].
A recent series of patients undergoing a trochanteric bursa injection for GTPS rated the pain 6.ane out of 10 in severity on a verbal numeric pain scale, and reported poor role (mean 50.1) on Harris hip scoring prior to the injection [6].
Following total hip arthroplasty (THA) 4–17% of patients report symptoms of GTPS [seven,8,9,ten]. Low dorsum pain, hip osteoarthritis [11] and rheumatoid arthritis [12], also announced to exist predisposing factors. Furthermore, in that location appears to exist a female preponderance, suggesting hip biomechanics including femoral commencement may also play a role [4].
Most cases are managed conservatively with simple analgesia, physiotherapy and corticosteroid injections. For refractory cases of GTPS where conservative measures have failed, numerous surgical techniques take been described [13].
Gluteal fascia transposition (GFT) has been described previously as a technique to decompress the greater trochanteric region [14]. To summarise, an 'H-shaped' incision is made in the fascia lata over the greater trochanter and the resulting flaps are folded dorsum on themselves and secured with sutures. This technique is also known as fascial windowing. The underlying bursa is and then excised.
Many studies looking at the efficacy of surgical techniques for GTPS exclude patients who have undergone previous THA [15, 13]. However, these patients may make upwards a significant proportion of refractory cases: Bakery et al. [14] report preliminary data to suggest that the aetiology of GTPS may have an upshot on outcome following GFT, with idiopathic cases appearing to accept a more satisfactory outcome than those with previous THA or revision.
This study aims to retrospectively evaluate patient reported outcomes and adverse events post-obit trochanteric bursectomy and gluteal fascia transposition, in relation to aetiology, in a consecutive case serial of patients treated by multiple surgeons at our establishment.
Patients and methods
Institutional approval was obtained for this written report. The BlueSpier (Bluespier, Droitwich, Worcester, U.k.) electronic database of clinical records was used to retrospectively place all patients who underwent bursectomy and GFT at our institution betwixt January 2010 and October 2022. Of the 62 procedures nosotros identified in 59 patients, nosotros excluded i patient who presented with a chronic infective bursitis following corticosteroid injection. All included patients had a clinical diagnosis of GTPS (defined by pain around the greater trochanter), had failed conservative treatment (defined as the return of symptoms following at least one successful corticosteroid injection, physiotherapy or both), and had been symptomatic for over one year at the fourth dimension of surgery.
The clinical records of patients were reviewed and the following data recorded: age; gender; duration of symptoms; underlying aetiology (idiopathic, ipsilateral THA, bilateral THA, ipsilateral full genu arthroplasty, traumatic, rheumatoid arthritis); presence of low back pain or ipsilateral hip osteoarthritis; previous surgery for GTPS; complications; any further procedures carried out since the index GFT.
We sent postal questionnaires to 58 eligible patients regarding 61 fascial transpositions (three patients experienced bilateral GTPS) at a median of 34 months postoperatively (range 9–77). In the absenteeism of a specific validated outcome tool, the following patient reported outcome measures were included: patient satisfaction score; ten cm visual analogue score referring to current level of pain (0–100, 0 representing no pain); Oxford hip score [xvi] (OHS; with a score of 0 representing worst function, and 48 best function); Likert scale duration of pain relief post-obit the functioning; Binary presence of pain when lying on affected side.
Satisfaction was measured according to the method described past Mahomed [17]. This scale consists of iv items focusing on satisfaction with the extent of pain relief, improvement in ability to perform abode activities, recreational activities and overall satisfaction. The responses were scored on a stemmed Likert scale (Appendix one), with the scale score beingness the mean of the four parts and ranging from 25 (least satisfied) to 100 (most satisfied).
Missing data were completed where possible via telephone interview past one of the authors (ERW). The mean value commutation method was used when a maximum of one data betoken was not reported for an effect measure. IBM SPSS Statistics for Windows, v22.0 (IBM Corp; Armonk, NY) was used for statistical analysis. A Mann-Whitney U test was used to compare the event of surgical intervention betwixt cases with an idiopathic aetiology and those who had undergone previous THA. Pearson coefficients were used to make up one's mind if there was a correlation between the reported outcome scores.
Results
We received responses from 49 patients, regarding 52 (85%) bursectomy and gluteal fascia transposition procedures. Demographic information for the written report population are presented according to aetiology in Table one. Historic period differed significantly between the idiopathic group (median age 58) and THA group (median age 74), p < 0.05. The results of pre-operative pelvic radiographs and ultrasound scans (USS) are summarised in Tabular array 2. Manifestly AP radiographs were available for review in 44 out of 49 patients. The most prevalent aberration was the presence of a bony spur over the trochanter. No varus hips (neck-shaft bending <120°) were identified however at that place were two valgus hips in the idiopathic GTPS grouping (neck-shaft bending >140°). An additional pre-operative USS was performed for 38 patients, revealing signs of either trochanteric bursitis or gluteal tendinopathy in 36 cases, see Table 2. Responders and non-responders were not significantly different in median age, length of follow-up or female preponderance. However, ane patient in the THA grouping did not respond, compared to six in the idiopathic grouping. Both cases where the aetiology was unknown did not respond.
Prior surgery for GTPS had been undertaken in vi patients in the ipsilateral hip: two labral tear repairs; 2 fascial windowing; one Z-lengthening; one arthroscopic psoas repair. An additional procedure at the aforementioned time as bursectomy and GFT occurred in seven patients: two bony debridement of lateral flare; two abductor reattachment; i psoas release; one repair of short external rotators; one osteophyte removal.
Outcomes
At a median of 34 months follow up, median visual analogue score (VAS) of 52 responses was 53 (interquartile range 10–75). Only four patients reported being completely pain free (VAS pain of 0). The median OHS was 25 (interquartile range 12–xl).
Pain lying on side
Figure 2A shows the responses of the total patient group to the question, 'Do you get pain lying on the affected hip?'. Of the 48 responses completed, 37 (77%) continued to have hurting lying on their side following GFT.
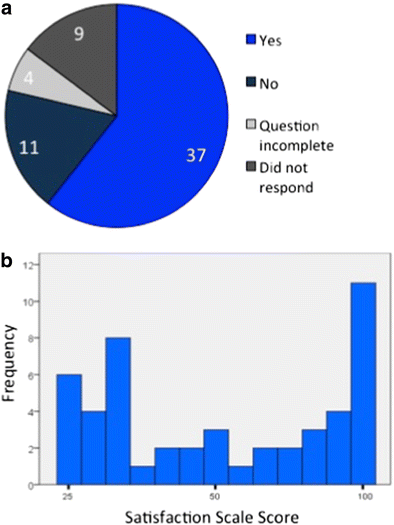
a Answers of all 61 patients to the question 'Do you become pain lying on the affected side?' at a median of 34 months post-obit gluteal fascial transposition and bursectomy. Question incomplete = no reply given; Did not respond = patients who did not return the questionnaire. b Frequency of satisfaction calibration scores amongst 52 patients who responded. The lowest score is 25 and the highest score is 100, signifying the well-nigh satisfaction
Satisfaction
The results of the 52 responses to our satisfaction survey are displayed in Fig. 2b. The distribution of scores was bimodal and symmetrical with a median satisfaction calibration score of 62.v (interquartile range 37.v–93.75) and modes at 100 and 37.five.
Pain relief
Figure 3 shows patient responses to the question 'Following your operation, for how long did you lot have hurting relief before your symptoms returned?'. Of 51 responses, 11 written report no relief at all; in comparison, 9 were still pain free at follow-upwards. Nineteen cases were hurting free for a twelvemonth or more.
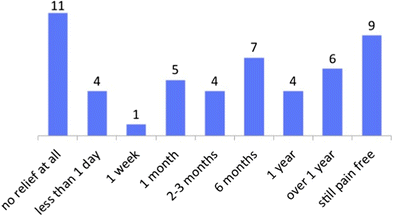
Length of pain relief following operation, for 51 patients who responded to the question, 'Post-obit your functioning, for how long did you have pain relief earlier your symptoms returned?'
Complications
Complications arose after eight of 61 operations in seven patients as follows: three significant post-operative haemorrhage; 1 haematoma; 2 wound infections; one persistent wound infection requiring multiple debridement operations and prosthetic joint infection; one required revision of GFT and LARS ligament (Corin, Cirencester, United kingdom of great britain and northern ireland) augmented tendon repair due to persistent pain. A further seven hips required additional operations for GTPS following the index fascial transposition: 2 LARS ligament augmented gluteal tendon repairs, two revision THA, 2 psoas releases, one excision of bony spur.
Outcome past aetiology
Postoperative VAS, OHS and satisfaction scores were compared for those with idiopathic aetiology and those with GTPS following THA (Fig. 4). Median satisfaction scores were 37.v post-obit THA vs. 87.5 for idiopathic cases (p = 0.006); median VAS were 73 THA vs. xx, idiopathic (p = 0.005); median OHS were 15 THA vs. 35 idiopathic (p = 0.015).
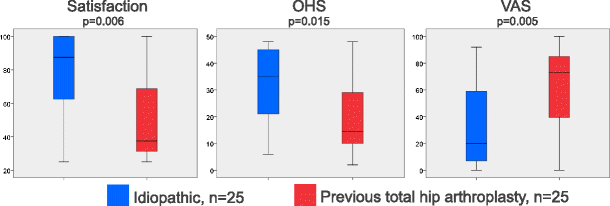
Satisfaction scale scores, visual analogue scoring (VAS) and Oxford hip scoring (OHS) analysed by aetiology of greater trochanteric pain syndrome (GTPS). Medians are shown (bars), with boxes showing interquartile range and whiskers showing range. p < 0.05 was deemed a significant difference in median scores on Mann Whitney U testing
Although idiopathic cases tended to be younger, satisfaction scores, VAS and OHS of respondents were not associated with age, gender, the presence or absence of low back pain or osteoarthritis in the same hip using regression assay. It is not possible to know whether previous surgery was associated with significantly worse outcome measures due to the small sample size.
Reliability of outcome measures
In that location was significant correlation betwixt satisfaction scoring, VAS and OHS (p < 0.001 for all cases). At that place was positive correlation between satisfaction and OHS (r = 0.62), and a negative correlation between OHS and VAS (r = −0.902), and satisfaction and VAS (r = −0.701). All patients who answered that they were still pain free had VAS scores of 20 or lower, suggesting reliability of the different event measures used.
Give-and-take
We written report a wide variation in outcomes following bursectomy and GFT, suggesting that this surgical intervention does not consistently produce a reliable outcome for refractory cases of GTPS. A disappointingly large number of patients in our case series were dissatisfied with the results of surgery, which is compounded by the relatively low overall median Oxford hip score of 25 (0 worst, 48 all-time) revealing the disabling nature of this condition, despite a class of conservative therapy and surgical intervention.
Numerous alternative surgical procedures attempt to treat patients with GTPS including open and arthroscopic bursectomy, iliotibial band Z-lengthening, open up or arthroscopic tendon repair, and trochanteric osteotomy [xiii]. In contrast to some other surgical methods, GFT aims to decompress the greater trochanter with excision of the bursa tissue. Whether the fascia is a key contributing crusade in the pathoaetiology of GTPS is all the same unknown.
To our noesis there has simply been one previous study reporting outcomes of bursectomy and GFT [14]. In comparison with this previous study, our results are disappointing. Approximately half of patients in our study were satisfied with their issue, compared with 75% in the previous study. Our results show that postoperative satisfaction, pain scores and OHS were significantly worse in cases with previous THA compared to idiopathic cases. With these patients making upwards 40% of cases in our series, our data add to those presented by Baker et al. [xiv], and are of significance because a consistent and major exclusion factor in studies of event following surgery for GTPS is previous ipsilateral THA [13, 15].
We hypothesised that the departure in result between idiopathic cases and those following THA may be related to differences in the underlying pathology or age; however, we were non able to identify pathological differences on the ground of ultrasound scanning. Similarly, although idiopathic cases were significantly younger, age did not correlate to whatsoever measure of issue, suggesting that advancing age did not account for the poor outcomes of fascial release after THA. In our series, only v of 25 cases had altered femoral kickoff following THA, suggesting cases following THA do non necessarily occur due to altered hip biomechanics. Futurity research might uncover differences in the pathology of THA and idiopathic cases of GTPS. In the meantime, nosotros suggest that patients with GTPS post-obit THA should be appropriately counselled about the poor effect of gluteal fascial release and bursectomy.
Early complications in both studies were reported in 13% of patients. Although about complications in our series were easily treated such as postal service-operative bleeding, haematoma and superficial infection, nosotros report 1 devastating prosthetic joint infection. In addition, a notable proportion of patients require further surgery for GTPS suggesting their pain was not improved; a finding not previously reported for this functioning. Complications reported in other surgical techniques for GTPS announced to be similar in nature [13] but have varying rates. Similarly, other studies study substantial rates of re-operation [13, eighteen].
Alternative surgical management, notably gluteal tendon repair, has been associated with better outcomes [19, 20]. In 72 patients with GTPS undergoing gluteal tendon repair, ninety% had no or minimal pain maintained at six and 12 months [twenty]. In these reports, a specific diagnosis of gluteal tendinopathy was identified on MRI, suggesting that surgery targeted at a specific pathology may be more effective. Even so, arthroscopic bursectomy without fascial release also appears to take encouraging outcomes at mid-term follow-up [18, 21] with low VAS scores at 2 years post-operatively, in patients with clinical features of GTPS.
Interpreting the electric current literature is complicated by the range of underlying pathology which is not always described, the departure in natural history between de novo and recalcitrant GTPS, the lack of specific diagnostic criteria and a lack of a specific tool to measure outcomes in GTPS; every bit such, widely varying outcomes are reported. However, common to many reports is the exclusion of cases with previous THA. The overall poorer outcomes in our study of GFT for GTPS compared to studies of other surgical techniques may exist explained by this difference.
A recent systematic review revealed a lack of testify to inform the management of GTPS [13]. For bourgeois measures, 4 randomised controlled trials have revealed pocket-size but temporary symptomatic relief following corticosteroid injections, and shockwave therapy. The evidence base of operations for patients with recalcitrant GTPS who have non responded to the usual conservative measures is limited to small case series, with variable success reported [thirteen]. We propose that whatsoever more invasive surgical treatment method should be superior in non only effect just besides length of symptomatic relief. In our case series, at median follow-upwards of 34 months, 41% retrospectively reported being pain-complimentary for one yr, but only four patients were pain free (VAS of 0) at time of follow-upwardly. To our cognition no prospective studies have directly compared surgical treatments with conservative measures. Such a trial is required, especially in the setting of refractory GTPS where it is important to know if surgery is superior to the continuation of non-operative measures.
Our retrospective case series is limited by a lack of baseline patient reported result measures. However, it has a relatively large sample size compared to other case series of surgical interventions for GTPS [14]. Nosotros were unable to identify whether physiotherapy was used as an adjunct to surgery in the cases in this series. The complications we written report are important to note if surgical intervention is existence considered for this condition. This study also importantly reports outcomes beyond the usual clinical follow upwardly period for this patient grouping, and beyond that reported in other studies.
Decision
We report overall poor outcomes following GFT and bursectomy for patients with refractory GTPS. The meaning complications and rates of farther surgery are apropos and are comparable to those reported in studies of other surgical methods for GTPS. Nosotros note significantly worse outcomes in those who have undergone previous THA, compared to idiopathic cases. Patients with previous THA are an of import group of patients, who commonly undergo surgical treatment for refractory GTPS but are excluded from other studies. Where cases of GTPS remain refractory to treatment with standard conservative measures such as corticosteroid injection (which tend to produce merely temporary symptomatic relief) we notation the urgent need for a trial comparing specialist conservative direction with targeted surgery in terms of length and degree of efficacy.
References
-
Fearon AM, Scarvell JM, Neeman T, Cook JL, Cormick Due west, Smith PN (2013) Greater trochanteric pain syndrome: defining the clinical syndrome. Br J Sports Med 47(10):649–653. doi:10.1136/bjsports-2012-091565
-
Fearon AM, Cook JL, Scarvell JM, Neeman T, Cormick W, Smith PN (2014) Greater trochanteric pain syndrome negatively affects work, concrete activity and quality of life: a case control study. J Arthroplast 29(2):383–386. doi:10.1016/j.arth.2012.ten.016
-
Klauser AS, Martinoli C, Tagliafico A, Bellmann-Weiler R, Feuchtner GM, Wick M, Jaschke WR (2013) Greater trochanteric pain syndrome. Semin Musculoskelet Radiol 17(ane):43–48. doi:ten.1055/s-0033-1333913
-
Segal NA, Felson DT, Torner JC, Zhu Y, Curtis JR, Niu J, Nevitt MC (2007) Greater trochanteric pain syndrome: epidemiology and associated factors. Arch Phys Med Rehabil 88(8):988–992. doi:10.1016/j.apmr.2007.04.014
-
Chowdhury R, Naaseri South, Lee J, Rajeswaran Thousand (2014) Imaging and management of greater trochanteric hurting syndrome. Postgrad Med J xc(1068):576–581. doi:ten.1136/postgradmedj-2013-131828
-
Park KD, Lee WY, Lee J, Park MH, Ahn JK, Park Y (2016) Factors associated with the event of ultrasound-guided trochanteric Bursa injection in greater trochanteric pain syndrome: a retrospective accomplice study. Hurting Physician xix(4):E547–E557
-
Iorio R, Healy WL, Warren PD, Appleby D (2006) Lateral trochanteric pain post-obit primary total hip arthroplasty. J Arthroplast 21(two):233–236. doi:x.1016/j.arth.2005.03.041
-
Sayed-Noor AS, Sjoden Go (2006) Greater trochanteric pain afterwards total hip arthroplasty: the incidence, clinical effect and associated factors. Hip Int 16(three):202–206
-
Farmer KW, Jones LC, Brownson KE, Khanuja HS, Hungerford MW (2010) Trochanteric bursitis afterwards total hip arthroplasty: incidence and evaluation of response to treatment. J Arthroplast 25(2):208–212. doi:ten.1016/j.arth.2009.02.008
-
Genth B, Von Düring G, Von Engelhardt LV, Ludwig J, Teske West, Von Schulze-Pellengahr C (2012) Analysis of the sensory innervations of the greater trochanter for improving the treatment of greater trochanteric pain syndrome. Clin Anat 25(viii):1080–1086. doi:ten.1002/ca.22035
-
Collee Yard, Dijkmans BA, Vandenbroucke JP, Cats A (1991) Greater trochanteric pain syndrome (trochanteric bursitis) in depression dorsum hurting. Scand J Rheumatol twenty(iv):262–266
-
Raman D, Haslock I (1982) Trochanteric bursitis--a frequent cause of 'hip' pain in rheumatoid arthritis. Ann Rheum Dis 41(6):602–603
-
Reid D (2016) The management of greater trochanteric pain syndrome: a systematic literature review. J Orthop xiii(i):15–28. doi:10.1016/j.jor.2015.12.006
-
Baker RP, MacKeith SAC, Bannister GC (2005) Gluteal fascial transposition for trochanteric bursitis. Hip Int 15(4):212. doi:10.5301/HIP.2008.1621
-
Drummond J, Fary C, Tran P (2016) The outcome of endoscopy for recalcitrant greater trochanteric pain syndrome. Curvation Orthop Trauma Surg 136(11):1547–1554. doi:ten.1007/s00402-016-2511-z
-
Dawson J, Fitzpatrick R, Carr A, Murray D (1996) Questionnaire on the perceptions of patients about total hip replacement. Bone Articulation J 78(two):185–190
-
Mahomed N, Gandhi R, Daltroy L, Katz JN (2011) The self-administered patient satisfaction scale for chief hip and knee arthroplasty. Arthritis 2022:591253. doi:10.1155/2011/591253
-
Larose C, Guanche CA (2012) Paper 28: arthroscopic treatment of recalcitrant greater trochanteric bursitis with minimum two-year follow upwardly. Arthroscopy 28(vi, Suppl 2):e59–e60. doi:10.1016/j.arthro.2012.04.034
-
Voos JE, Shindle MK, Pruett A, Asnis PD, Kelly BT (2009) Endoscopic repair of gluteus Medius tendon tears of the hip. Am J Sports Med 37(4):743–747. doi:x.1177/0363546508328412
-
Walsh MJ, Walton JR, Walsh NA (2011) Surgical repair of the gluteal tendons: a written report of 72 cases. J Arthroplast 26(8):1514–1519. doi:ten.1016/j.arth.2011.03.004
-
Baker CL Jr, Massie RV, Injure WG, Savory CG (2007) Arthroscopic bursectomy for recalcitrant trochanteric bursitis. Arthroscopy 23(eight):827–832. doi:ten.1016/j.arthro.2007.02.015
Writer information
Affiliations
Corresponding writer
Ideals declarations
Conflicts of interest
Eve Robertson-Waters, James Berstock, Michael Whitehouse and Ashley Blom declare no conflict of interest.
Funding
This inquiry did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors.
Appendix 1. Patient Questionnaire and Satisfaction Questions
Rights and permissions
Open up Access This commodity is distributed nether the terms of the Creative Commons Attribution 4.0 International License (http://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided you lot give appropriate credit to the original author(s) and the source, provide a link to the Artistic Commons license, and indicate if changes were fabricated.
Reprints and Permissions
Nearly this article
Cite this article
Robertson-Waters, E., Berstock, J.R., Whitehouse, M.R. et al. Surgery for greater trochanteric hurting syndrome afterward total hip replacement confers a poor upshot. International Orthopaedics (SICOT) 42, 77–85 (2018). https://doi.org/x.1007/s00264-017-3546-7
-
Received:
-
Accepted:
-
Published:
-
Issue Date:
-
DOI : https://doi.org/10.1007/s00264-017-3546-vii
Keywords
- Hip
- Hurting
- Bursitis
How Long Is The Actual Surgery For Trochanteric Bursitis Wirh Gluteus Repairs,
Source: https://link.springer.com/article/10.1007/s00264-017-3546-7
Posted by: jacksonstinst.blogspot.com


0 Response to "How Long Is The Actual Surgery For Trochanteric Bursitis Wirh Gluteus Repairs"
Post a Comment